Addressing health inequalities: the role of speech and language therapy
This page provides guidance on health inequalities and the role of speech and language therapists in mitigating inequalities in their services.
(Last updated June 2023)
Back to the health inequalities index page for case studies and other resources.
Who is this resource for?
This resource is for individual speech and language therapists (SLTs), speech and language therapy teams and services, researchers and/or educators to use in speech and language therapy curriculums. It is relevant for those working in the NHS, independent practice, research, higher education institutions (HEIs) and all other non-NHS settings.
This resource aims to develop understanding across the profession of health inequalities and how to take action to ensure equality and equity, and that the profession is meeting the needs of the populations we serve.
Please see our glossary for definitions of key terms that are used throughout this guidance.
What are health inequalities?
“Health inequalities are avoidable, unfair and systematic differences in health between different groups of people. There are many kinds of health inequality, and many ways in which the term is used. This means that when we talk about “health inequality”, it is useful to be clear on which measure is unequally distributed, and between which people”. (The King’s Fund, 2022).
“Health inequalities result from social inequalities. Action on health inequalities requires action across all the social determinants of health.” (Marmot, 2010, p15).
What does it mean?
Health inequalities are about differences in the status of people’s health, care and opportunities to lead healthy lives.
The link between the social conditions in which a person lives and health inequalities has been understood and documented often; the 2010 report ‘Fair Society Healthy Lives’ by Sir Michael Marmot (2010) is clear that progress towards a fairer society is marked by the magnitude of health inequalities in the population.
The follow-up report (Health Equity in England: The Marmot Review 10 Years On, 2020), laid bare the widening gap in health inequalities in England, with life expectancy reducing in deprived areas outside London for women and in some regions for men. The World Health Organisation defines the social determinants of health as “the non-medical factors that influence health outcomes.”
The term covers many different health inequalities that can arise because of the circumstances and factors that affect peoples’ lives. Health inequalities involve differences in:
- life expectancy
- healthy life expectancy
- avoidable mortality
- long-term health conditions
- prevalence of mental-ill health
- access to and quality of health services
- behavioural risk factors (e.g. smoking, poor diet)
- wider determinants of health (e.g. income, housing, education, transport, work and environment).
Some groups of people who share certain characteristics may be more vulnerable to health inequalities than others, because they are under-served by the healthcare system (‘under-served groups’).
“In England, health inequalities are often analysed and addressed by policy across four types of factors:
- socio-economic factors, for example, income
- geography, for example, region or whether urban or rural
- specific characteristics including those protected in law, such as sex, ethnicity or disability
- socially excluded groups, for example, people experiencing homelessness.”
(The Kings Fund, 2022)
People experience different combinations of these factors, outside their direct control, which has implications for the health inequalities that they are likely to experience. There are also interactions between the factors which is important to consider. This can lead to unfair, and avoidable differences in their health, the care they receive and the opportunities they have to lead healthy lives.
As Napier et al (2014) state: “The systematic neglect of culture in health and health care is the single biggest barrier to the advancement of the highest standard of health worldwide” (Napier et al, 2014, p 1608).
These factors are unlikely to impact on a person one at a time, it is far more likely that the impact will be felt by many of these factors interacting, both in parallel and in sequence over time.
As an SLT how much do you know about how these factors affect all your service users?
Health inequalities, under-served groups and the equality, diversity and inclusion (EDI) agenda
Those experiencing health inequality are often from particular under-served groups. The equality, diversity and inclusion agenda should strive to serve such groups to mitigate health inequality.
Increasingly, research is evidencing the differential outcomes experienced by under-served groups:
- Black and ethnic minority patients experience differential (often poorer) outcomes in healthcare, and people from ethnic minority groups are more likely to report being in poorer health than white counterparts (The King’s Fund, 2021).
- People who are LGBTQ+ are more likely to experience health inequalities, caused by societal norms that prioritise heterosexuality as well as outright discrimination and stigma (Zeeman et al, 2018).
- Those who are homeless are vulnerable to health inequalities, arising from intertwined adverse social and economic conditions (Stafford and Wood, 2017).
- People with learning disabilities face health inequalities and are at particular risk of premature death (LeDeR, 2020).
- Those living in socio-economically disadvantaged areas may be more likely than those living in affluent areas to experience multiple health problems in adulthood (multi-morbidity) though the causal factors require examination (Olutende, Mse, Wanzala and Wamukoya, 2021).
- Looked after children, who predominantly interact with social workers, may have their health needs overlooked, contributing to health inequalities (Bywaters, 2009).
- There are inequalities in the health of people who belong to traveller communities, more so than almost any other group in the UK (van Cleemput, 2010).
- Those who lack the skills, do not have connectivity or devices, lack confidence or motivation to or find accessing digital platforms challenging may also be at risk of health inequalities (NHS digital, 2022).
What leads to health inequalities?
As outlined in the previous sections, the associated variables, causes and pathways to health inequalities are varied and complex. Members are encouraged to use the references and resources hub to explore these further.
Here, we outline some key factors related to discrimination that can contribute to health inequalities.
Institutional biases
Different types of institutional biases exist, for example systemic racism, homophobia, transphobia, classism or ableism.
Typically, these biases arise from the design of our healthcare systems and the paradigms which they operate under, which may foster and perpetuate discriminatory beliefs and values (Hui, Latif, Hinsliff-Smith Chen, 2020). Thus, a system and workforce develop which are unable to deliver equitable care (Bailey et al, 2017).
‘Systemic’ or ‘institutional’ racism refers to “how ideas of white superiority are captured in everyday thinking at a systems level: taking in the big picture of how society operates, rather than looking at one-on-one interactions.” (O’Dowd, 2020).
In healthcare systems, institutional racism may contribute to health inequality for Black and minority ethnic populations – this is inextricably linked with the anti-racism agenda.
Examples of system-wide issues that may perpetuate health inequalities are:
- Our health care systems being underpinned predominantly by one model of illness and disability (ie ‘western’ medicine, medical models of disability) which render service users operating outside of this vulnerable to disempowerment and leads to inequitable care.
- See examples of religious beliefs relevant to understanding and experiencing health and healthcare in Swihard, Yarrarapu and Martin (2021).
- See specific perspectives from under-served groups on approaches to speech and language therapy in Roulstone et al (2015, p 143-145).
- Historically poor representation of people from ethnic minority backgrounds, women, who are LGBTQ+ or with disabilities in clinical research, potentially leading to recommendations that are not appropriate for different populations, which can result in inadequate clinical guidance (see eg Smart and Harrison, 2017).
- Biased educational materials and curricula meaning clinicians are not taught how to deliver appropriate care to those from marginalised groups (see example of speech and language from Pillay and Kathard, 2015), or the development of assessment materials lacking sensitivity and representation of marginalised groups therefore creating barriers to engagement.
- Failure to adequately fund a workforce and services required to meet the needs of diverse populations such as overcoming language and cultural barriers, for example not allocating funding for interpreters or development of diverse resources (Piacentini, O’Donnell, Phipps, Jackson and Stack, 2018).
- Ethnicity and gender disparities in position, prestige and pay among healthcare staff have been described in research, affecting, for example, hiring practices and career progression of ethnic minority staff (Milner, Baker, Jeraj and Butt, 2020).
Implicit bias
A clinician’s implicit bias may also contribute to health inequalities. Implicit bias is the making of “associations outside conscious awareness that lead to a negative evaluation of a person on the basis of irrelevant characteristics such as race or gender.” (FitzGerald and Hurst, 2017).
Research has shown that healthcare professionals may possess implicit biases which can influence health outcomes. A systematic review concluded that healthcare professionals exhibit implicit bias at the same degree to the mainstream population. These biases may influence clinical decision making, and the level of care offered to service users (FitzGerald and Hurst, 2017).
Studies have documented examples of healthcare professionals with biases toward under-served groups such as:
- Traveller communities (Frances, 2013)
- People of colour (Hall et al, 2015)
- LGBTQ+ people (Sabin, Riskind and Nosek, 2015)
- Disabled people (VanPuymbrouck, Friedman and Feldner, 2020).
As an SLT, are you cautious about making direct assumptions or judgements of service users who both share or do not share your own culture, race, ethnicity or religion?
Going unresolved, a clinician’s implicit bias may therefore create inequality in healthcare. Changing this is unreservedly imperative and is an element of becoming anti-racist, anti-homophobic, anti-transphobic or anti-ableist, and an ally to those from other under-served groups.
What is the SLT role in health inequalities?
Interventions to tackle health inequalities need to reflect the complexity of how health inequalities are created and perpetuated, otherwise they could be ineffective or even counterproductive.
This guidance looks firstly at the broader role of speech and language therapists and then more specifically at the typical factors that impact on a service users’ experience, and how an SLT might contribute to reducing or mitigating any health inequalities that arise. There are also some interesting observations on the impact of allied health professionals (including SLTs) on health inequalities in a recent rapid review (Ford et al, 2021).
The NHS Constitution requires all staff to contribute towards providing fair and equitable services for all and help to reduce inequalities.
The COVID-19 pandemic highlighted existing health inequalities (see, for example, Katikireddi et al, 2021). As we moved through the pandemic, we noted an increasing focus on population health and health prevention. This is an opportunity to highlight the role of speech and language therapy in contributing to better population health and reducing health inequalities. See this King’s Fund article for a definition and discussion of population health.
NHS England’s health inequalities improvement programme developed Core20PLUS5, a national approach to inform action to reduce healthcare inequalities at both national and system level in England. Its purpose is to define populations where accelerated improvement in healthcare services is required, along with 5 key clinical areas, for both adults and children. Integrated Care Boards in England are focussed on addressing health inequalities in these target groups. We have produced two infographics to show how SLTs contribute to these focus areas. You can use them to highlight the role of SLTs wherever it is appropriate, to discuss in team meetings or in the MDT or with students on placement for example.
Broader role of SLTs
A crucial part of the speech and language therapist’s role is understanding not just the ‘norms’ of development and communication breakdown in English, but also the norms of development and communication breakdown in other languages and amongst those with disabilities– as well as thorough understanding of the implications of food modification for those with dysphagia.
An SLT must be able to provide personalised and equitable care to all service users who require it, thus understanding each individual’s preferred language, culture, religion, family setup, attitudes toward their health status, beliefs on approaches to play, language or rehabilitation is imperative. Decisions regarding telehealth approaches should thus also be personalised, and the SLT should carefully consider access to digital/telehealth and digital inclusion. Having well-planned, accessible, equitable, and appropriate care pathways, resources, assessment materials and workforce are all essential to mitigating health inequalities.
SLTs may also provide universal services or public health services which may not involve directly working with individuals with speech, language, communication or swallowing needs, or directly about their speech, language, communication or swallowing needs. There is a role for SLTs in addressing health inequalities through this work too. For example, training early years services providers in language enrichment may support a wider range of children than the number which would attend clinics. These resources could be targeted in areas where people may be more likely to face barriers in accessing healthcare, such as areas of greater socio-economic deprivation. There may also be a role in supporting speech and language therapy service users to access other support especially those who are more vulnerable to health inequalities, for example, working with people with a learning disability to understand the importance of dental hygiene. Services may be designed to incorporate these offers and mitigate health inequalities. Again, these services must be well-planned and with resources that are suitable and accessible for the population it is aiming to serve.
SLTs must develop ‘cultural humility’ and commit to working reflexively across their careers. SLTs will need to constantly adapt their practices to best meet the communities that they work with.
Inclusive speech and language therapy
As highlighted earlier in this guidance, whilst the reasons for health inequalities are vast and complex, evidence has shown that discrimination is an important underlying factor that can contribute to health inequalities.
Institutional and implicit bias can result in a lack of equitable and appropriate speech and language therapy thus contributing to health inequalities. SLTs should be providing fair, culturally and linguistically appropriate and inclusive services to all.
To support the profession to do so, the RCSLT and members have produced a range of resources, all of which can be found in our health inequalities resources page.
Specific roles of SLTs
Access to services
- SLTs should consider the impact of services being accessible and especially to potentially under-served groups, for example, do they have the confidence and skills to navigate their local healthcare system; can they travel to them or are there language barriers?
- SLTs are able to help a service user with communication needs and health literacy, (see RCSLT’s Inclusive Communication guidance and information on Communication Access UK). This can support services to meet the requirements of the Accessible Communication Standard and supporting reasonable adjustments for people with communication impairments.
- SLTs must also consider when an interpreter is required, in particular new HCPC standards from 1st September 2023 place particular emphasis and requirements on the assessment and planning of interventions in the service user’s home language (see and guidance on working with Interpreters and on bilingualism).
- SLTs need to assess whether digital poverty is impacting on access to services delivered via telehealth (see RCSLT’s telehealth guidance section on digital inclusion).
- SLTs should consider possible groups of people who may not present to NHS services, for example homeless people or those seeking asylum. Does your service have any plans or initiatives to specifically support individuals such as those who are homeless, to access the service?
- SLTS should consider the design of services and the offer of targeted and universal services, and whether options other than targeted/individual therapy would increase access to SLT expertise.
Health status
- SLTs can understand any co-occurring health needs and be aware of health needs of particular under-served groups in planning appropriate care.
- SLTs can take account of the prevalence and incidence of clinical conditions in the population in general, and if there is any known research about specific under-served groups.
Quality and experience of care, for example, levels of service user satisfaction
- SLTs can ensure they understand the service user’s experience and social factors that affect them. This can form a part of your initial assessment (see RCSLT guidance on assessment) and could include seeking views from service users in the planning of services, see RCSLT guidance on children’s services for example).
- SLTs can personalise care for individuals from different cultures, ethnicities, family setup, languages and socio-economic situations and intellectual ability from their own.
- SLTs can consider the cross-cultural differences in which families access speech and language therapy services and attend regular appointments, ie, older siblings or elder family members attending with children.
- SLTs recognise that adherence to expert dietary guidelines will vary due to food beliefs and practices which will impact on dysphagia management.
- At a personal level the service users’ preference, taste, psychological state is considered.
- At an interpersonal level, the patterns of the household, food preparation and habits of significant others are investigated.
- At a community level the food availability and prices which could influence the accessibility of modified food and food choices are also taken into account.
- For those offering universal or public health services, are the stakeholders you are working with satisfied/have a good experience and do they consider that the service is equitable and appropriate for all?
Behavioural risks to health
- SLTs can support service users to understand health risks and choices through Reasonable Adjustments to their communication needs.
- SLTs support early years development in their awareness of diverse cultural and social communication environments.
- SLTs can support general health promotion campaigns e.g. referral to a smoking cessation service for a parent who smokes when discussing their child’s glue ear, through the rapport they develop with service users and their carers eg Make Every Contact Count.
Wider determinants of health
- SLTs can take account of impacts of deprivation and socio-economic inequalities in managing their caseload e.g., arranging appointments in the community, where the majority of their funding is targeted.
- Funding and service design may also need to be considered as to how to maximise impact and avoid inequalities, e.g., considering your universal and targeted offers
- SLTs can signpost to appropriate services, both in healthcare and non-healthcare e.g., debt advice.
- SLTs can understand co-occurring intellectual disabilities and the structural barriers people with learning disabilities face in accessing health services, including diagnostic overshadowing and institutional ableism.
- SLTs can consider appropriate ‘did not attend’ policies to take account of ability to attend or language barriers or in planning interventions appropriately taking account of potential service user factors, e.g., homelessness.
- SLTs can consider appropriate “was not brought” policies to take account of ability of parents or carers to bring children to appointments that take account of service user factors, such as ability to pay for transport.
- SLTs can facilitate success in education/employment as protective factors for health by assessing and treating communication disorders.
SLT and service role in collecting and analysing data
- An additional role of the SLT is evaluating and monitoring your caseload or population you serve to ensure you are aware of the needs of everyone you are serving through your practice. The key to this is collecting data about your service users robustly and routinely. This should include basic information about the service users, eg demographic information such as age, gender, ethnicity and diagnoses (see Equality Act 2010) and outcome measures.
- Data can then be analysed in conjunction with information you have about the local population, and prevalence/incidence of clinical conditions to see if ‘theory’ matches ‘reality’.
- For those offering universal services or services outside of individualised care, you can still measure impact and outcomes and use this for monitoring purposes. You may find our guidance on measuring outcomes outside of individualised care useful.
- Informally gathered information is also helpful – if you do not have access to central data, maybe reflect with your team – what kind of proportion of your caseload do you think might not have English as their first language? Be careful not to make assumptions, but anecdotal information like this might be a useful starting point.
- The government’s ‘Early Years Health Development Review Report: The Best Start for Life, A vision for the 1001 Critical Days (2021)’ cites that “good quality datasets are essential to identifying and eliminating the greatest inequalities. Reviewing what data is collected and ensuring it is collected in a way that is both efficient and punctual and that it is correctly recorded will make a substantial difference.” (p 101). Read the full government report.
- SLTs can engage with learning from premature deaths and specific current data gathering approaches e.g., reporting any death of a child (4 years plus) or person with a learning disability for a review through the Learning Disabilities Mortality Review (LeDeR) programme (LeDeR, 2021) (see the LeDer website)
- Collecting data can sometimes be a sensitive factor for some patients, especially with regard to ethnicity, gender and sexual orientation. The NHS has developed a Sexual Orientation Monitoring Information Standard which you may wish to refer to.
- See the health inequalities resources for more information on gathering data in this area.
Members can log in to view related RCSLT guidance on:
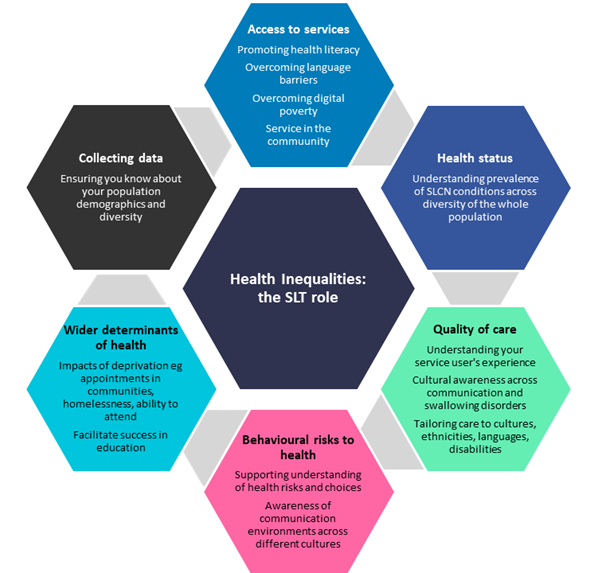
Summary of the SLT role
References and acknowledgements
This is the full list of references for our health inequalities guidance, further reading and acknowledgements to the members who helped during the development and updating of this resource.
- Bywaters, P. (2009) Tackling Inequalities in Health: A Global Challenge for Social Work. British Journal of Social Work, 39 (2), 353-367. DOI: 10.1093/bjsw/bcm096
- Classism (2021) About Class. [Online] [accessed 7 July 2021]
- FitzGerald, C. and Hurst, S. (2017) Implicit bias in healthcare professionals: a systematic review. BMC Medical Ethics, 18 (19). DOI: 10.1186/s12910-017-0179-8
- Ford, J. Aquino, M. R. J., Ojo-Aromokudu, O., Van Daalen, K., Gkiouleka, A. Kuhn, I., Turner-Moss, E., Thomas, K., Barnard, R. and Strudwick, R. (2021) Rapid Review of the Impact of Allied Health Professionals on Health Inequalities. University of Cambridge. Online. [Accessed 9 July 2021]
- Hall, W. J. Chapman, M. V., Lee, K. M., Merina, Y. M., Thomas, T. W. et al (2015) Implicit Racial/Ethnic Bias Among Health Care Professionals and Its Influence on Health Care Outcomes: A Systematic Review. American Journal of Public Health. 105 (12), e60-e76. DOI:10.2105/AJPH.2015.302903
- Hui, A., Latif, A. Hinsliff-Smith, K and Chen, T. (2020) Exploring the impacts of organisational structure, policy and practice on the health inequalities of marginalised communities: Illustrative cases from the UK healthcare system. Health Policy. 124 (3), 298-301. DOI: 10.1016/j.healthpol.2020.01.003
- Iacobucci, G. (2020) The BMJ Interview: Victor Adebowale on systemic racism in the NHS. BMJ, 371. DOI: 10.1136/bmj.m4111
- Katikireddi, S. V., Lal, S.,Carrol, E. D., et al (2021) Unequal impact of the COVID-19 crisis on minority ethnic groups: a framework for understanding and addressing inequalities. Journal of Epidemiology and Community Health. DOI:10.1136/jech-2020-216061
- The King’s Fund (2022) What are health inequalities? [Online] [Accessed 25 November 2022]
- The King’s Fund (2021) My role in tackling health inequalities: a framework for allied health professionals. [Online]. [Accessed 7 July 2021]
- The King’s Fund (2021) The health of people from ethnic minority groups in England. [Online] [Accessed 7 April 2021]
- Learning Disabilities Mortality Review (LeDeR) Programme (2020) Annual Report 2020. [Online] [Accessed 7 July 2021]
- Marmot, M. (2010) The Marmot Review: Fair Society, Health Lives. [Online] [Accessed 15 April 2021]
- Marmot, M., Allen, J., Boyce, T., Goldblatt, P and Morrison, K. (2020) Health equity in England: The Marmot Review 10 years on. [Online] [Accessed 18 May 2021]
- Milner, A., Baker, E., Jeraj, S. and Butt, J. (2020) Race-ethnic and gender differences in representation within the English National Health Service: a quantitative analysis. BMJ Open, 10:e034258. doi: 10.1136/bmjopen-2019-034258
- Napier, A. D. et al (2014) Culture and health. Lancet, 384(9954), 1607-39. doi: 10.1016/S0140-6736(14)61603-2.
- NHS Digital What we mean by digital inclusion [Accessed 25 November 2022]
- National Institute for Health Research (2022) . National Institute for Health Research. [Online] [Accessed 21 June 2023]
- O’Dowd, M. G. (2020) Explainer: what is systemic racism and institutional racism? [Online] [Accessed 6 April 2021]
- Olutende, M. O., Mse, E., Wanzala, M.N. and Wamukoya, E. K. (2021) The Influence of socio-economic deprivation on multi-morbidity: a systematic review. European Journal of Physical Education and Sport Science, 6(12), DOI: 10.46827/ejpe.v6i12.3656
- Piacentini, T., O’Donnell, C., Phipps, A., Jackson, I. and Stack, N. (2018) Moving beyond the ‘language problem’: developing an understanding of the intersections of health, language and immigration status in interpreter-mediated health encounters. Language and Intercultural Communication, 29 (3), 256-271.
- Pillay, M. and Kathard, H. (2015) Decolonizing health professionals’ education : audiology and speech therapy in South Africa. African Journal of Rhetoric, 7(1).
- Roulstone, S. E. et al (2014) Evidence-based intervention for preschool children with primary speech and language impairments: Child Talk – an exploratory mixed-methods study. Programme Grants Appl Research, 3(5). DOI:10.3310/pgfar03050
- Sabin, J. A., Riskind, R. G. Nosek, B. A. (2015) Health Care Providers’ Implicit and Explicit Attitudes Toward Lesbian Women and Gay Men. American Journal of Public Health, 106(9), 1831-1841.
- Scope (2021) Disablism and ableism. [Accessed 9 July 2021]
- Smart, A. Harrison, E. (2017) The under-representation of minority ethnic groups in UK medical research. Ethnicity & Health, 22 (1), 65-82. DOI: 10.1080/13557858.2016.1182126
- Stafford, A. and Wood, L. (2017) Tackling Health Disparities for People Who Are Homeless? Start with Social Determinants. International Journal of Environmental Research and Public Health. 14 (12), 1535. DOI: 10.3390/ijerph14121535
- Stonewall UK (2021b) Glossary of items. [Accessed 9 July 2021]
- Swihart, D. L., Yarrarapu, S. N. S. Martin, R. L. (2021) Cultural Religious Competence In Clinical Practice In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing.
- Van Cleemput, P (2010) Social exclusion of Gypsies and Travellers: health impact. Journal of Research in Nursing. 15 (4), 315-327. DOI: 10.1177/1744987110363235
- VanPuymbrouck, L., Friedman, C., Feldner, H. (2020) Explicit and implicit disability attitudes of healthcare providers. Rehabilitation Psychology. 65(2), 101–112. DOI: 10.1037/rep0000317
- Yeager, K. A., Bauer-Wu, S. (2013) Cultural humility: essential foundation for clinical researchers. Applied Nursing Research. 26(4), 251-6. doi: 10.1016/j.apnr.2013.06.00
- Zeeman, L., Sherriff, N., Brownse, K., McGlynn, N., Mirandola, M. et al (2019) A review of lesbian, gay, bisexual, trans and intersex (LGBTI) health and healthcare inequalities. European Journal of Public Health. 29 (5), 974-980. DOI: 10.1093/eurpub/cky226
Further reading
For information on Research and Evidence relating to the broader topics of Anti-racism, diversity and inclusion please see our dedicated anti-racism pages
You can also read our Inclusive Practice Journals round-up – offering summaries of latest research on EDI issues and speech and language therapy.
The World Health Organisation have published a ‘Global report on health equity for persons with disability’ outlining recommendations for country-level actions to address gaps.
For additional supporting resources and background reading see the Health inequalities resources page.
Acknowledgements
With thanks to the following RCSLT members who have provided feedback during development of this information.
Ilyeh Nahdi
Aydan Suphi
Sean Pert
Nabiah Sohail
Sahar Nashir
Sarah Spencer
Sally Morgan
Lindsey Thiel
Dharinee Hansjee
Julie Marshall
Dave McDonald
Katherine Pritchard
Toria Kilsby
Rachael Middle
Alex Wormall
Alpana Marwaha
Rachael Middle
Anna Raby
Sophie Woodford
Matthew Horton
Kerry Corley
Pat Mobley
Glossary
Ableism
Ableism is discrimination in favour of non-disabled people (Scope, 2021). See Scope for further discussion of both ableism and disablism.
Bias
Having a bias is an inclination or prejudice for or against one person or group, especially in a way considered to be unfair.
Classism
“Classism is differential treatment based on social class or perceived social class. Classism is the systematic oppression of subordinated class groups to advantage and strengthen the dominant class groups.” (Classism, 2021)
Cultural humility
“A lifelong process of self-reflection and self-critique whereby the individual not only learns about another’s culture, but one starts with an examination of her/his own beliefs and cultural identities.” (Yeager and Bauer-Wu, 2013)
Digital inclusion / exclusion
Digital inclusion describes the ability of all individuals to access digital, digital exclusion thus describes what can happen if one does not have access. Some sections of the population are more at risk of digital exclusion than others, these include people: in specific age groups (such as older people), with disabilities, in lower income groups or without a job living in rural areas, in social housing or homeless people, whose first language is not English (NHS Digital, 2020). Read more about digital inclusion in our Telehealth guidance.
Disproportionality
Describes when an individual or a group of individuals is dis/ advantaged in one way or another that is not representative of what would be expected as a whole.
Ethnicity
Ethnicity is defined variably, however it is often used to group people with long, shared significant experiences, such as “culture, language, history or set of traditions”. Ethnicity may be the “state of belonging to such a group”. (Cambridge dictionary online, 2022). It is not synonymous with “race”.
Implicit bias
“Implicit biases involve associations outside conscious awareness that lead to a negative evaluation of a person on the basis of irrelevant characteristics such as race or gender.” (FitzGerald and Hurst, 2017)
Institutional bias
Bias induced or embedded within a system or institution (ie not individual), operating at a systems level. Can include institutional or systemic racism, homophobia, transphobia, classism, ableism.
Intersectionality
Used to discuss individuals’ experience of multiple and intersecting identities/social factors, often those that are related to forms of oppression, prejudice or discrimination (Crenwshaw et al., 1995).
Race
Adopting a critical approach, ‘race’ is a social construct that has been used to privilege white people, and for them to exert power over others. In this regard, ‘race’ manifests as groupings of people based on physical characteristics, such as skin colour. Racialised individuals are people who are not white and do not have white privilege – they will often have a common experience of racism. Racial identity is thus still important to many.
Social deprivation / social exclusion
The concepts of social deprivation and social exclusion share a similar focus on the inability of individuals to participate fully in the life of their community or society. The measurement of social deprivation has tended to emphasise a lack of material or financial resources that contributes to a lack of social participation, whereas measures of social exclusion have emphasised the lack of participation to a broader range of social, cultural, and political activities (Levitas et al., 2007). From Chandola & Conibere (2015).
Socio-economic status
Typically this describes the social standing of an individual, though can be measured variably. One example of measuring socio-economic status may be household income, but could also include occupation and education status.
Transphobia
“The fear or dislike of someone based on the fact they are trans, including denying their gender identity or refusing to accept it. Transphobia may be targeted at people who are, or who are perceived to be, trans.” (Stonewall, 2021b)
Under-served groups
In the context of healthcare and health research, an under-served group describes a population or community with shared characteristics that have historically been disadvantaged in receiving adequate health care or quality/volume of research, to an equal standard of the ‘mainstream’ population. The National Institute of Health Research said in 2020 that common characteristics of under-served groups
“can include:
- Lower inclusion in research than one would expect from population estimates.
- High healthcare burden that is not matched by the volume of research designed for the group.
- Important differences in how a group responds to or engages with healthcare interventions compared to other groups, with research neglecting to address these factors.”
In this section
Health inequalities case studies
Examples of how SLTs have addressed health inequalities
Health inequalities resources and references
Further reading to continue your learning on health inequalities
 Download as PDF
Download as PDF

